|
RADICAL PROSTECTOMY SURVIVAL HANDBOOK
Part 1
Part 2 Part 3
by
Ron Voss & Janet Olson
Second Edition - 2000
(Reproduced at Phoenix5 with permission. All "editor notes" are by the authors.)
What Cancer Cannot Do
Cancer is so limited…
It cannot cripple love,
It cannot shatter hope,
It cannot corrode faith,
It cannot destroy peace,
It cannot kill friendship,
It cannot suppress memories,
It cannot silence courage,
It cannot invade the soul,
It cannot steal eternal life,
It cannot conquer the spirit.
- From The Circle, Source unknown
THE RADICAL PROSTATECTOMY SURVIVAL
HANDBOOK
This is not necessarily a medically accurate paper. It is a collection of experiences by people who have been diagnosed with various stages of Prostate Cancer and have been treated by Radical Prostatectomy. Its purpose is to help you anticipate what you might encounter and to be prepared. It is from the patient's point of view. Your experience may, and probably will, vary.
I'm sorry to hear that you are a member of this club, but you are in good company, with many warm, generous people out there to help and support you. I will list some resources at the end of this document.
My Story
It all started when I was 53 and went to a new doctor for a routine physical. My old doctor had never done a PSA test before, and this one felt that it probably was about time to have one along with all the other lab work. This was about the first week in March, '97. About a week later, I received a call, on a Saturday, no less! He told me that everything looked good, except that I had a high PSA (over 7, it should be less that 3.5). He also said that he did not feel confident investigating this and felt that I should see a specialist. He tried to reassure me that, because it was my first PSA, a high reading might not mean anything.
I contacted Doctor Turek, a urologist I had previously worked with at UCSF, who also tried to reassure me that, because of previous recent testing, it was probably nothing to worry about, but, that I still should go ahead with an ultrasound guided biopsy, and he was recommending me to Doctor Shinohara who has done thousands of these procedures, and was probably one of the best in the world. It was the end of March, and early Friday morning I was at UCSF for the ultrasound. Doctor Shinohara said that he could not see anything significant, except that half of the prostate looked a bit darker than the rest- my first clue. He went ahead and took 12 samples from different areas, and we, Jan and I, took them down to the lab for analysis which would take about three days. To make a long story shorter, all the doctors were out of the area until the first of May, which meant that we were on pins and needles for two weeks. As you've undoubtedly figured out by now, the results came back positive, and I did indeed have cancer of the prostate.
By the middle of June, near my birthday, I'd seen two oncologists, Doctor Joseph Presti and Doctor Peter Carroll, both at UCSF-Mt. Zion Cancer Center, and had a Trans-Rectal MRI. At this time I made a decision and scheduled surgery with Doctor Presti.
Jumping Ahead
The doctors, according to the pathology reports and three years of follow-up PSA tests, were able to remove all of the cancer! This does not necessarily mean that I am 100% free of this disease only time will decide that.
I had almost no problems with the catheter, and it was not even uncomfortable. Actually it was kind of convenient. I could just drain it whenever I felt like I wanted to, or even have Jan, my wife, do it for me. I found that I only needed to secure the catheter at the end where the valve is, first with a layer of tape on my thigh, then a layer through the crotch of the 'V', and then a layer over the whole 'V' to keep it from twisting. The first time I removed the tape, I realized that I should have shaved that
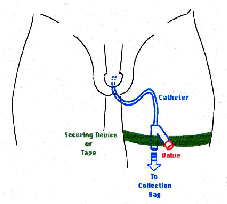 area! Later on, Jan purchased a foam and Velcro catheter securing device which just wrapped around my thigh - No Tape - and by using the 'V' in a similar manner I was able to secure it quite solidly, (see drawing - click to enlarge in new window).
area! Later on, Jan purchased a foam and Velcro catheter securing device which just wrapped around my thigh - No Tape - and by using the 'V' in a similar manner I was able to secure it quite solidly, (see drawing - click to enlarge in new window).
As Richard Miller wrote to me,"I'm not wearing my heart on my sleeve, but my bladder on my leg."
My energy levels jumped by leaps and bounds every day following the first few days after surgery and any serious discomfort quickly began to fade after the first week. It plateaued after that, and then the long process of getting back to normal began.
Pre-Surgery Thoughts and Tips
Books
To start off with, I have several recommendations for books and a cassette that might be of help. The first is titled, The Prostate: a Guide for Men and the Women who Love Them by Patrick C. Walsh and Janet Farrar Worthington, published by Johns Hopkins University Press. This will help you to understand your disease and exactly what the surgery involves.
The second, a book and a tape, is titled, Love, Medicine & Miracles and is written by Bernie S. Siegel, M.D. It was even recommended by Ann Landers! It deals with how your attitude can effect your personal outcome with this and any serious health problem .
The third is a new book which was published in September of 1997. It is titled, A Revolutionary Approach to Prostate Cancer written by Aubrey Pilgrim and published by Sterling House, 440 Friday Rd. I Pittsburgh, PA 15209. Over 20 MD's contributed chapters and articles to the book. It has contributions from several survivors and it will cover all the current treatment options.
Private Room
If you can afford it, and have a significant other who is willing to stay with you, by all means, ask for a private room. Having Janet stay with me for the first few nights and act as my advocate really helped (this was an Idea suggested to me by Geoffrey Bauman). Just keep in mind how exhausting this can be to your partner and that he/she might need to escape for a while or even for a night to get some real rest in order to return refreshed to again care for you. I granted my wife, Janet, sainthood for all she did for me, and I believe that I understated how I felt.
Get-a-way
Again, if you can afford it and because you don't know where the end result of this surgery will leave you (incontinent, impotent), plan a long weekend just before your surgery to make a memory with your significant other. The memory of it will help carry you through if you start to feel overwhelmed or depressed.
Janet, my wife, and I reserved a room at The Fantasy Inn at Lake Tahoe, CA. The place was noted for having theme rooms such as Graceland, Romeo and Juliet, Rain Forest, etc. The only suite that was available was the Arabian Nights, but it was a lot of fun. I'm only sorry that I didn't have time to rent some good costumes like Aladdin and Jasmine to complete the effect. We went for a dinner/dance sunset cruise on the lake, hiked, played, had great meals at good restaurants, saw a stage play, and thoroughly enjoyed each other's company. It was money well spent for the memories we gathered.
Do It!
Tapes
Because of the information in the Bernie Siegel book, I started working with my psychologist, who provided me with Post-Op and Pre-Op hypnosis tapes.
The Pre-Op tape was 15 minutes long. I had it played to me during the first stage of anesthesia, it dealt with controlling bleeding in the abdominal area of surgery , and with staying calm and positive during surgery; it had no wake up message at the end.
The Post-Op tape I had played immediately after surgery, it served to control bleeding, to control pain, and to affirm that the healing process had already begun. Additionally, its wake up message suggested that I would awaken feeling refreshed, thirsty, and hungry, I'm not sure if the last two items were a such a good idea, as I was allowed no water or food during the first day.
In addition to those tapes, I also recorded a 90-minute cassette of music that I knew would be soothing to me, avoiding anything that might have a negative or minor tone to it, while including music that had special meaning, such as a song by Michael Franks that reminded me of how much I love my wife.
When I scheduled my surgery , I asked the surgeon and the anesthesiologist if it would be possible to have these tapes played in the proper order for me: the Pre-Op tape, the music tape (to continuously loop until the end of surgery), and then the Post- Op tape. The surgeon went so far as to say that if the tapes couldn't be played to me through my Walkman and headphones, he would play the music for everyone to hear. It turned out that I was able to use the headphones.
You ask,"Why go to all this trouble?" Well, I'm told that I was the first patient they had seen, to be wheeled out of surgery with a smile on his face. When I awoke, I knew I was already beginning to heal. Also, the anesthesiologist was able to use less anesthesia than would normally be required for this type of operation, and I was able to use less pain medication than most people. Is all this attributable to the tapes? I can't prove it but I think the answer is, Yes!
Consumer Reports On Health
In the August '97 issue of "Consumer Reports On Health", there is an article titled "How to prepare your mind and body for surgery". Within this article is a section called, "Psyching yourself up for surgery". They suggest that you use any of several methods ( guided imagery tapes, massage, meditation, yoga, etc.) to "alleviate potentially harmful stress before, during and after surgery. Stress raises blood pressure and heart rate, increasing the risk of cardiac complications. It may also prevent patients from eating or sleeping properly, delay wound healing and deplete the body's defenses against infection." "Stress also makes you more sensitive to pain. Pain can prevent you from moving your muscles or your bowels, from breathing deeply, or even from coughing to clear your lungs, all of which can slow recovery and increase the chance of complications". All of which you will probably experience to one degree or another.
I have listed the resources that they suggest at the end.
Chair
Because the surgery will, to some degree, rearrange your lower anatomy, and, because the catheter passes through that area, sitting can be a real pain in the butt!
I found that, when I first came home, I could not sit up straight, nor, because of sutures in my abdominal wall, could I lie down flat. Luckily, I had a recliner that enabled me to relax in a semi-folded position. A few days later I was able to fully recline in bed, but it was a bit of a stretch.
Several suggestion that were made to me were:
1 - Purchase or borrow a recliner. You'll need it for about a month.
2 - Purchase or borrow a rocking chair. The rocking action constantly shifts your weight, thus preventing fatigue and pain at anyone spot.
3 - If you cannot do either of the above, try sitting in a very cushioned chair or sofa, or on pillows, with your feet on an ottoman or the coffee table and slouch down like when you were a kid at a Saturday matinee, (Don't let your mother see you doing this as she will yell at you to sit up straight!). Make sure you place pillows behind your back for support. Having something under your knees to keep them slightly bent also helps.
Pillow
A friend, Kate Hutchinson, suggested this, and, boy, was I glad she did! Take a pillow with you when you are ready to come home from the hospital and keep it near
you at all times!! Hold it tightly over your incision whenever: you are in a car or plane and accelerate, decelerate, or hit a bump; you sneeze (absolutely the worst thing); you laugh, or cry (which I found myself doing frequently for things like someone having sent me a cookie bouquet, or trying to thank someone for their concern and kindness). The Pillow will soon become one of your best friends.
Coat hanger
If you don't have a plastic coat hanger, buy one. An idea that Jan had, to facilitate the hanging of the catheter collection bag along side the bed, was to take a plastic coat hanger and insert it between the mattresses sideways, leaving a small part of the bend at one end of the hanger sticking out from the side of the mattress, you can then hang your night collection bag on this. It has turned out to be very convenient.
Brush
I have found that a long-handled bath brush can enable you to shower by yourself because you can reach your back and your feet. Make sure that someone is with you for your first shower just for safety purposes.
Shower Safety Bar
If you can, install a safety bar in the shower. It gives you something to hang on to at first and a great sense of security later. The one I installed is epoxy coated and exactly matches the wall tile, making it unobtrusive. Make sure it is securely attached to the studs in the wall or some other backing because, if you slip or fall, it will have to support your full weight plus the inertia of the fall. Unless you really know what you are doing, I would recommend having it installed by a professional.
Pre-Surgery Jitters
About two days before the surgery, I was walking around the house saying, "What the hell am I thinking of! I feel fine and have no symptoms of any illness. So, I'm planning to go to the hospital, where someone can split me open like a ripe watermelon, scoop some of my insides out, glue me back together, slap me on the back, and tell me to go home and that my life will never be the same! No Way, Jose'! Let's go back to Tahoe until after Thursday!" (the RP date). By the next day, I knew that this was something I WAS going to do, because I also knew what the future consequences might be, and I liked those much less. There are success stories. Of course it still remains to be seen, in the long term and between PSA tests, if I will continue to be one of them. One can only hope.
Surgery
July 17, 1997
Once I was unconscious it was relatively easy.
Post-Surgery
Sutures
There are three kinds of sutures commonly used in surgery. Gut type sutures which must be snipped and removed after about a week. Staples, metal sutures, that must also be removed after about a week. Dissolving sutures, which will just dissolve and falloff in a few weeks.
Strips of a special tape over the the top of dissolving sutures, which falloff at the same time the sutures dissolve, are sometimes used to help reinforce these.
Ask your surgeon what he uses, so that you will know what to expect.
Dry Mouth
I was not allowed any fluid until the next morning following surgery and suffered with severe dry mouth. The nurses provided glycerin swabs and sponge swabs dipped in water but, for me, it was not sufficient. I was never in any real danger, but I felt as if I was going to suffocate. My uvula, that thing that hangs down in the back of your throat, was swelling and was causing me to have a swallowing reflex. My mouth being so dry, the uvula would stick and cause my breathing passage to close, blocking the airway. I could consciously hold the airway open, but upon falling asleep, it would close waking me up immediately. I was having wake/sleep cycles of about 20 seconds, making for a VERY long night/day. Finally, Janet was able to get someone to understand enough of my distress to get my doctor to come over. He looked at my hands, noticed they were swollen too, and had my IV volume reduced by 50%. Within the hour my uvula returned to normal and I could, FINALLY, get some sleep... 24 hours after coming out of surgery!
Pain Control
Pain is a natural by-product of any surgery, and this is major surgery. So, before you find yourself faced with pain control, discuss your options and their side effects with your surgeon and your anesthesiologist. Make sure you understand what they have told you. Make a decision. Then, make sure that both of these doctors understand and agree to your wishes.
Painkillers
The morphine drip, which I had control over, worked wonderfully well. The problem I had was when I came home without it and began taking Vicodin.
1 - All narcotics slow down the recovery of the intestine and so increase the incidence of gas.
2 -The doctors will probably disagree with me but I feel that the Vicodin can affect you psychologically.
I have a friend who has been through similar abdominal surgery twice and found Vicodin to act like a depressant after taking it several days, and the Morphine acted like a hallucinogenic. She didn't mind this during the day - probably even enjoyed it - but at night it terrified her.
My experience was that the Vicodin made me feel more than a bit psychotic and even on sensory overload, somewhat like an autistic person might feel: certain colors, sounds and touches were … painful. I noticed that this began in the hospital when I was on the just the Morphine because I did not even want to have the TV on or music playing; I just wanted quiet!. I was just glad that I could realize it was the painkillers that were causing this effect and that it would wear off - which it did, in about six sleepless hours.
I was left with a choice: I could continue to take the prescribed Vicodin which is supposed to have a lesser effect on the intestines' recovery than others; I could change to something like Tylenol and Codeine which could slow the intestines more but with different side effects; or just go over to something not as effective but, in my case, with no known side effects such as Advil. I opted for the Advil route after checking with my doctor, who, I believe, thought that I must be crazy to try and manage this level of pain with no more than someone would take for the average severe headache. On a one to ten scale, I would say that it kept the pain in the three to five range.
Bloating
Due to anesthesia and the use of pain killers, the intestines tend to shut down, and it can take anywhere up to about five days for them to come back on line. The problem is that the residue in the intestines continues to break down, and, in so
doing, produces gas which, because the intestines are still asleep, cannot be moved out of the body in a timely fashion. So, I blew up like a dirigible and expected to explode like the Hindenburg and go down in flames. This was the most painful part of my surgery because not only did I have extensive gas cramps but the extra pressure was pushing rather hard upon the surgery area which was still VERY sore. I tried everything in the hospital they had to throw at it, which wasn't much, suppositories, Mylanta and Milk of Magnesia. When I returned home I tried Gas-X and Papaya Enzyme, still no use. What seemed to work the best was TIME, although a suggestion by one of my nurses seemed to help a bit, that was to lie on my left side, very difficult in the first 48 hours, and go to sleep.
John Bush, a friend from The Circle newsgroup said that he was told that they would not give him laxatives or stimulants since there could be a danger of bursting the bowel, like over-inflating a balloon. He says, "I'm not a doctor, just relating my own understanding".
Jim Hornaday, who you'll read about later, has a friend who found that walking seemed to be a BIG help.
Another option that seemed to help was to take very small bites while eating and chew them into nothingness.
One other thing I would suggest, eat only foods that you know are easy for you to digest, I think the head dietitian at my hospital went to Hamburger University... and didn't graduate!
The bottom line is, we did survive.
Temperature Control
It took about a week till I my body was able to effectively regulate my temperature. I would be freezing one moment, put blankets on and warm up only to have it swing the other way and find myself in a pool of sweat.
It was a greater problem at night. I felt that I couldn't move off the area that I
had soaked in perspiration because then I would get cold and begin to shiver - very painful. So, Jan figured out that she could slip a dry bath towel under me so that I did not have to get out of bed, which was painful, or become chilled. This way she did not have to change the bedding until the next morning, curing the problem and also didn't have to help me out of bed to change the bedding till morning.
Emotions
About a day after surgery I became an emotional yo-yo. Everything that was nice or good would start me crying - which wasn't a good idea considering the waves of pain it shot through my abdomen. I'd look at Jan and think about all she'd done for me", and start crying. Someone would send me flowers or a cookie bouquet… I'd start crying. About four days later, the problem was laughing and the more it would hurt the harder I would laugh. Sure glad I had my pillow with me. I began returning to normal after about two weeks.
Post-RP Depression
Post-surgical depression is quite common. If you think about it, you've been doing a lot of preparation of your body and mind to get ready for surgery. You can't keep those energy levels up forever, so once you've come through your ordeal, they drop - and you drop with them. The effects of the anesthesia and having had your body violated, work together to also cause psychological negatives. The good part is that this effect will fade as you start to get back on your feet and more toward a normal life.
Leakage
I began to have leakage around my catheter after about six days (not a problem,just inconvenient) and tried a product recommended to me by someone on PPML (Prostate Problems Mailing List - A Newsgroup found on the Internet). The product is 'Rejoice' and it is underwear with replaceable pads. Very comfortable and, unless you look closely, indistinguishable from normal. The waistband sits easily above the navel, thus avoiding the area of incision and has the added benefit of keeping the catheter in the comfortable 'S' shape of a sink trap, you know, down, up, down. Great Product.
I did have one minor complaint that I contacted the manufacturer about. After having put in a couple of pads, I found that the glue strip was so good that the pad would not separate from the boat (the pant's containment area) without leaving the glue strip behind and sometimes causing the pad's last layer to separate from the rest of the pad. The manufacturer suggested that I only use part of the glue strip, say a small area at the front and back or a small area in the middle, or not use the strip at all as one of the women in their office does. This seems to have solved the problem.
You may want to purchase the pants and pad, or some similar product, ahead of time, rather than having to scramble through your wife's supplies when you spring a leak, and from what I've been told, you will.
Dribble Effect
After having the catheter removed on August 6, 1997, I found that, although I
had reasonable continence, I suffered from what I call the Dribble Effect. Whenever I would be standing I could sense, drip, drip, drip. Not much volume, just a drop at a time. As long as I was seated or reclining, I had no problem. I discovered that, when I would go out for one of my three daily walks around the block, the dripping stopped. This soon re-emphasized what others had been telling me were the best recovery aids - Do your Kegels and Walk, Walk, Walk!
Serious Leakage
I had to return to the hospital for a cystoscopy and a bladder-neck dilation because my urinary flow had diminished to a drip. So, they put me back on the Foley for another 2 weeks. It improved the flow so much that I was ready to find some snow to write my name in - if it didn't all leak out before I got there.
I was wearing the "shorts with the extra padding", (don't tell Janet, she still thinks that she was seeing my real butt when I wore tight jeans), when I had one of those 'unexpected events' the next day. Luckily I caught it before I walked into Costco. I didn't realize that I was leaking and my pad had filled up and overflowed. I had to head home for a change of clothes and clean underwear. I was able to sit on a towel that I just happened to have in the car,
I began carrying an extra pad with me.
First Outing
Janet let me out for the first time one week after the surgery. I thought that we could walk around the block but she felt that just to the end of the block would be enough for the first outing. As usual, she knew better than I did and by the time we returned to the house my butt was dragging and I had to take a 45 minute nap to recover. But it was so nice to be out and it was such a beautiful, sunshine warmed day. I could hardly wait to get out into the garden - I guess that I would have to be able to reach the ground and get back up before that could happen.
Exercise
As I have always been a fairly physical person, the first things I wanted to do when began to feel better, two to three weeks post-RP, were: start working out; work in the garden; swim; do house maintenance; get my abdominals back in shape. I might have attempted some of these, except that the doctor explicitly said that I could not: lift anything heavier that ten pounds, do any strenuous exercise, or even drive for five to six weeks. And, believe me, Janet was right there to enforce those rules. I found that my body seemed to side with them, and against me, too!
Nerve Sparing
Doctor Presti was going to spare the nerve bundle on only one side of the prostate, but, because of the favorable results of an ER-MRI, he said, if it was possible and would not affect the outcome, he would try save them both - and he did! Even two weeks out of surgery, when the catheter was still in, I noticed that, when I would awaken in the morning, I was beginning to have very soft erections! I could hardly believe it! I didn't expect there to be any stirrings for over six months if at all!
I have a friend who did not have either nerve spared, but, two years later, he is beginning to notice that he is now getting some soft erections. It seems that it is possible, in some cases, for the nerves regrow themselves at a rate of up to only 1/8th of an inch a month. So, it is a slow process. But, it can happen. I am proof of it.
Nerve Sparing and Regrowth
About three months after surgery, I had my first visit with Dr. Tom F. Lue, Professor of Urology and Chief of Urology, at UCSF-Mt. Zion Medical Center, he is a specialist in erectile function. It turns out that he was also selected by one of the medical publications as one of the 100 best doctors in the country - if that means anything. He also has a great sense of humor.
While in his office and impressing him with my vast knowledge of the subject, I mentioned something about the regrowth speed of the nerve as being approximately 1/8th of an inch per month and he said, "I can see that you've been doing your homework, but were you aware that we can now significantly speed the regrowth of the nerve bundles?" He has been working on this for the past ten years, with success over the past four years, and had a paper coming out at the end of 1997 in the New England Journal of Medicine or the American Journal of Medicine, I can't remember which.
Sex: A Warning
Like any kid with a new toy, I wanted to try it out. My first experience was about 3-1/2 weeks post-surgery - thanks to a patient, understanding and loving wife. This was at my request, knowing full well that I would not be able to achieve a useful erection, and thinking that no one had ever mentioned this subject, so it probably wasn't important. I had one of the best orgasms, completely dry, that I can ever remember. But, I paid for it!
Later that day I began to have to urinate almost every one to two hours, around the clock. The areas where the lymph nodes and the prostate were removed became very painful again and sensitive to any pressure. I began to have a headache - all over my body. And, I had to start taking Advil again.
What happens is, during orgasm, the muscles in your abdomen contract quite strongly while the pleasure center of your brain is stimulated, cutting off most pain inputs. You don't feel it immediately, but it is like lifting a heavy object -which is a no- no!
The next day my semi-continence returned but the areas of surgery continued to be painful for a few days.
My suggestion, ask the doctor, and then proceed according to his instructions.
You Can Get Through This
No matter what you hear elsewhere, this is difficult, but you CAN get through it, especially with support of family and friends, a support group or a counselor. If at all possible, do not do this on your own! It is OK to ask for help. It is also OK to be frightened, sad, angry , etc. but don't keep it in, talk about it with whoever will listen (oops, sorry for being preachy.). Keep a positive attitude going in and KNOW that you are already beginning to heal the moment you come out of surgery. Be patient with yourself and with those trying to help you.
Health, Healing and Happiness,
Ron Voss
GO TO PART 2 THAT STARTS WITH
THE PARTNER'S PERSPECTIVE
|
|